Medically reviewed by
Harold H. Cameron, MD
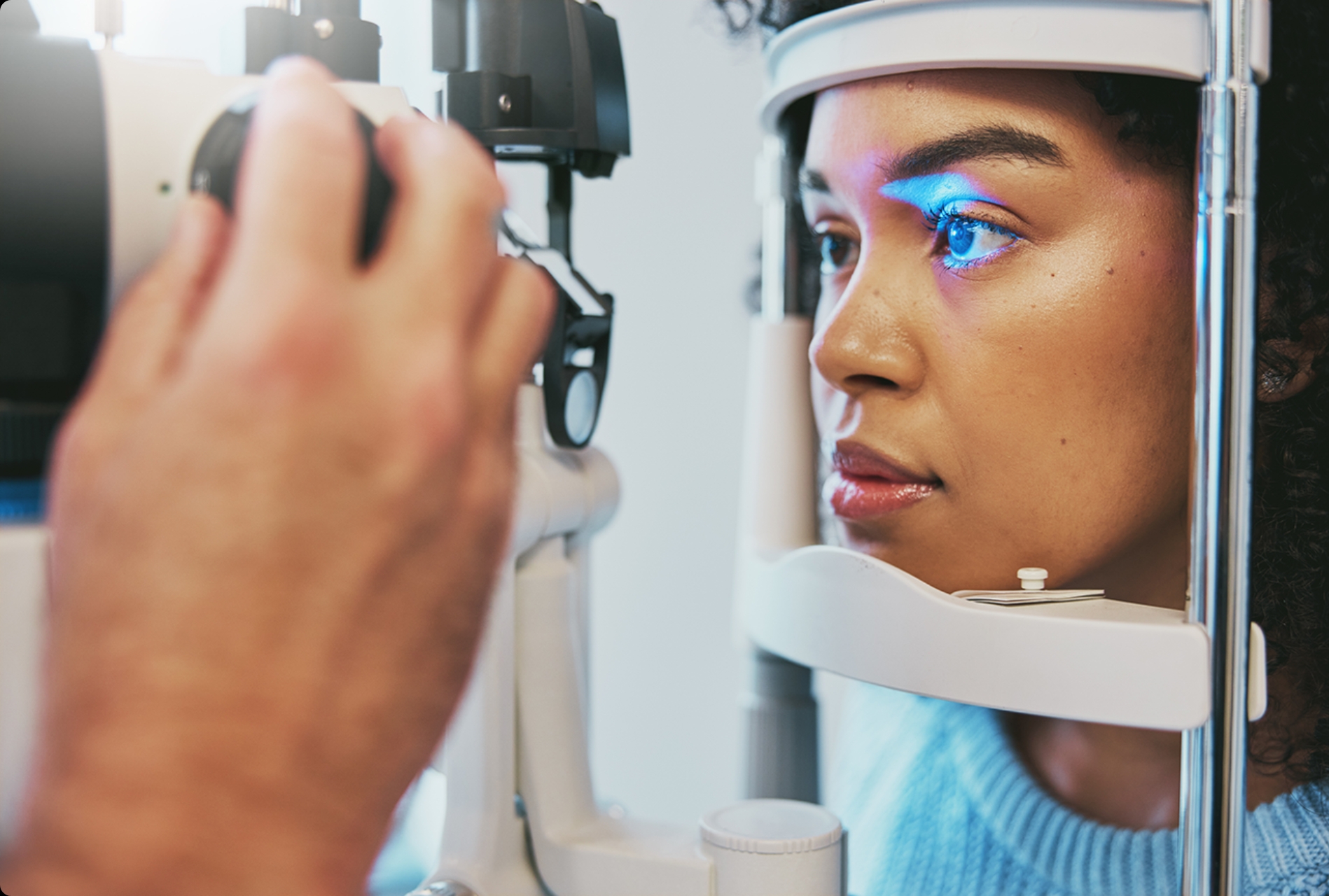
If you’ve been diagnosed with diabetes, you’re already adjusting to diet, exercise, and medication regimens your doctor prescribes. But you may not know that diabetes brings special dangers to your sight. These dangers can be detected and monitored through regular eye exams before you notice any symptoms.
Jump Ahead
- The Growing Diabetes Challenge
- Understanding Diabetes and Its Types
- What Does Insulin Do?
- How Eye Doctors Detect Diabetes
- Four Major Eye Diseases
- Prevention
The Growing Diabetes Challenge
The statistics are alarming. According to the most recent CDC data, approximately 38 million Americans (about 1 in 10 people) have diabetes. Even more concerning, 1 in 5 people with diabetes don’t know they have it. Nearly 98 million American adults have prediabetes, and more than 8 in 10 of them are unaware.
The disease has risen faster among Americans of Black and Hispanic origin, and rates continue increasing for people under 19. Diabetes affects people of all ages, making annual eye exams crucial for patients across the lifespan.

Understanding Diabetes and Its Types
Diabetes comes in three forms: Type 1, Type 2, and gestational diabetes. Gestational diabetes affects a small percentage of pregnant women and typically resolves after giving birth, though it increases the risk of developing Type 2 diabetes later.
Type 1 Diabetes
Type 1 diabetics lose the ability to make the insulin hormone, often after a viral illness damages cells in the pancreas that produce insulin. This form was formerly called juvenile diabetes but can develop at any age. Physicians typically detect it in general exams and treat it promptly.
Common symptoms include:
- Excessive thirst and drinking
- Constant need to eat
- Frequent bathroom use
- Fatigue
- Terrible breath
Type 2 Diabetes
Type 2 is the most common form, accounting for approximately 90-95% of all diagnosed diabetes cases in adults. In Type 2 diabetes, blood sugar rises to dangerously high levels. The pancreas makes more insulin to compensate but can’t keep up, as receptors for insulin on cells become desensitized to the hormone.
Type 2 usually begins later in life and proceeds silently, which makes regular dilated eye exams crucial. Your eye doctor may be the first person to identify diabetes, especially if you don’t have regular medical checkups.
What Does Insulin Do?
Understanding insulin’s role helps explain why diabetes affects your eyes:
First, insulin regulates blood sugar levels. Your body breaks carbohydrates down into glucose, a sugar that provides your primary source of energy. Insulin lets glucose in the bloodstream enter your cells.
Second, insulin helps you store excess glucose in the liver as glycogen. Between meals, when insulin levels drop, the liver sends glycogen back into the bloodstream as glucose.
If you have diabetes, glucose levels continue to rise after you eat because there’s not enough insulin to move it into your cells. Untreated high blood glucose can lead to complications including blindness, nerve damage, and kidney disease.
How Eye Doctors Detect Diabetes
No other place in your body reveals diabetes problems as easily as your eyes. Here’s why:
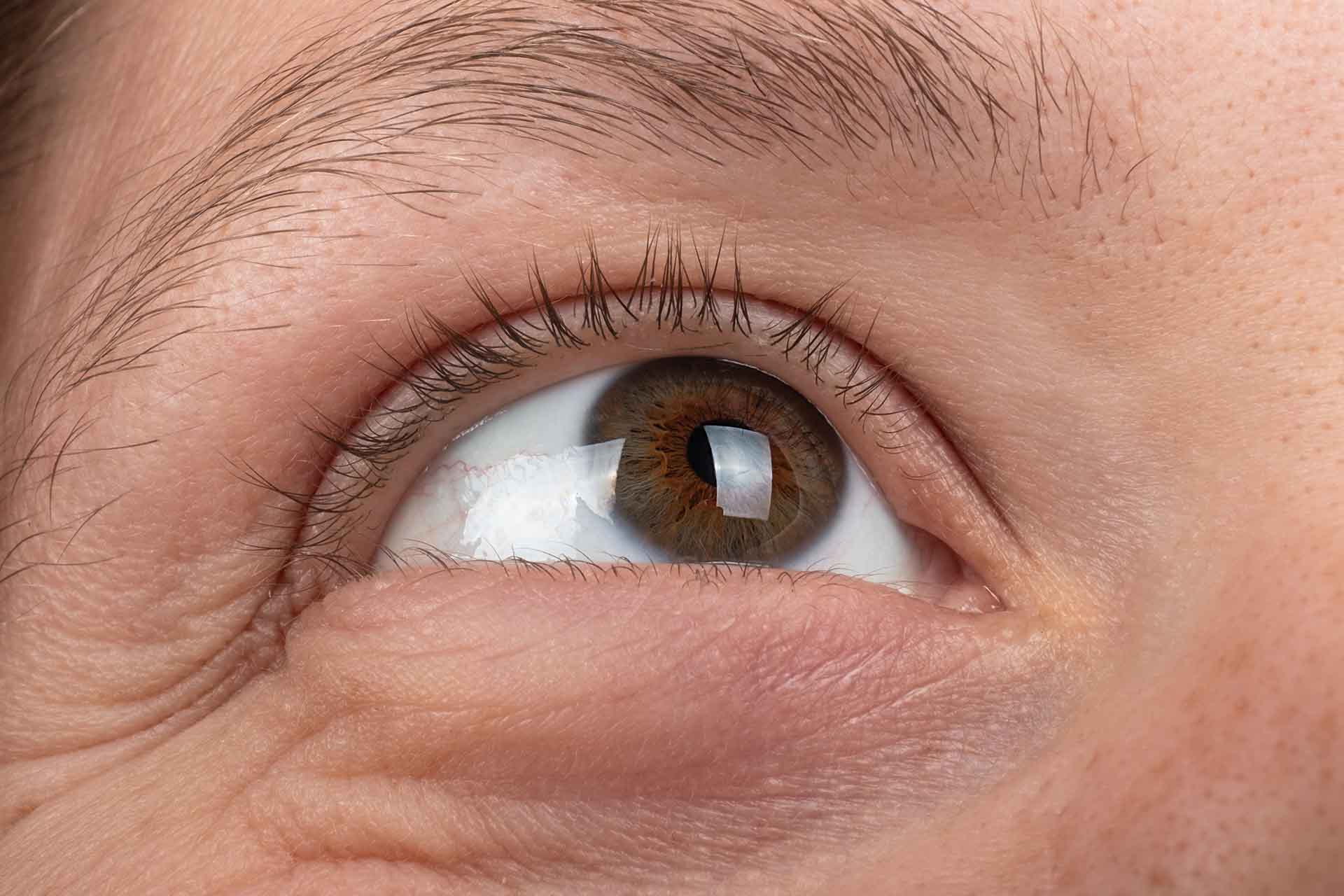
Water typically follows sugar into cells through osmosis. When blood sugar is high, a cell swells with excess water. The swelling and de-swelling of that cell eventually kills it. When a patch of cells in a blood vessel wall dies, pressure inside the vessel makes that portion of the wall balloon outward in what’s called a saccular aneurysm.
Eye doctors can see these aneurysms during a retinal exam. What’s happening in the eye is also likely occurring in other organs, but the eye provides the clearest window into these changes.
Four Major Eye Diseases Affecting People with Diabetes
1. Diabetic Retinopathy
Diabetic retinopathy progresses in stages and occurs when glucose damages blood vessels in the retina. Those vessels can swell and leak or close to prevent blood from flowing through. Sometimes abnormal blood vessels grow on your retina.
Non-proliferative diabetic retinopathy (early stage)
In this phase, blood vessels in your retina weaken. Tiny bulges stick out from the vessel walls, sometimes leaking or oozing fluid and blood into the retina. This stage has few symptoms and can often be managed with proper diabetes control.
Proliferative diabetic retinopathy (advanced stage)
Damaged blood vessels close off, causing the growth of new, irregular blood vessels in the retina. These new blood vessels can leak into the vitreous (the clear, jellylike matter that fills the center of your eye). You may notice blurriness or a sudden increase in size or number of floaters in your field of vision. Diabetics’ vision may grow foggy after a big meal, then clear up as blood sugar drops. One eye often responds differently from the other.
Can Diabetic Retinopathy Be Reversed?
The initial stages of diabetic retinopathy can be managed and progression slowed through proper glycemic control, diet, weight loss, and exercise. However, the damage done to the eye is usually permanent. If left too long, the disease cannot be reversed, and diabetic retinopathy remains a leading cause of blindness in working-age adults.
2. Diabetic Macular Edema
Diabetic macular edema (DME) occurs when leaking blood vessels cause fluid buildup in the macula, the part of the retina that controls our most detailed vision abilities.
It takes two forms:
- Focal DME: Abnormalities in blood vessels
- Diffuse DME: Widening or swelling of retinal capillaries
Treatments include:
- Anti-VEGF injections to reduce swelling
- Anti-inflammatory steroids
- Surgery (vitrectomy) to remove blood from the vitreous
3. Cataracts
Adults with diabetes are two to five times more likely to develop cataracts (a clouding of the natural lens) and at younger ages than people without diabetes. Cataracts grow faster in diabetics, particularly when levels of excess blood sugar increase.
4. Glaucoma
People with diabetes are twice as likely to get glaucoma, a group of diseases that permanently damage the optic nerve linking the eye to the brain. This risk makes regular eye exams even more critical for diabetics.
Diabetes-Related Eye Diseases Comparison
| Condition | What It Is | Key Warning Signs | Is It Preventable? |
|---|---|---|---|
| Diabetic Retinopathy | Damaged blood vessels in the retina that leak or close off | Floaters, blurred vision, dark spots, vision changes (often no early symptoms) | Yes – with blood sugar control and early detection |
| Diabetic Macular Edema | Fluid buildup in the macula causing swelling | Blurred or wavy central vision, difficulty reading | Yes – manageable with early treatment |
| Cataracts | Clouding of the eye’s natural lens | Cloudy or blurry vision, faded colors, glare sensitivity | Partially – progresses faster with poor blood sugar control |
| Glaucoma | Damage to the optic nerve from increased eye pressure | Often no symptoms until advanced; gradual vision loss | Yes – with early detection and treatment |
Prevention is Possible
Approximately 90 percent of diabetes-related vision loss can be prevented with early detection and proper management. Unfortunately, about 50 percent of diabetic patients don’t get the regular eye exams doctors recommend. Early detection is key, especially because patients often don’t detect changes in vision before the disease advances to a dangerous stage. Many people have no symptoms in the early stages of diabetic retinopathy.
Additional Considerations for People with Diabetes
Increased Infection Risk
Diabetics become more susceptible to infections (especially eye infections) and are slower to heal. This makes contact lenses more problematic if owners don’t clean them carefully and follow proper hygiene practices.
Insurance Coverage
Medical insurance typically covers eye exams for people with diabetes, so you don’t need separate vision insurance to get annual checkups. This makes regular monitoring more accessible and affordable.
Frequently Asked Questions About Diabetes & Eye Health
How often should people with diabetes get eye exams?
Everyone with diabetes should have a comprehensive dilated eye exam at least once a year, even if vision seems fine. Those with Type 1 diabetes should begin annual exams five years after diagnosis, while those with Type 2 diabetes should start immediately upon diagnosis. Pregnant women with diabetes may need additional exams throughout pregnancy.
Can diabetic retinopathy be reversed?
The initial stages of diabetic retinopathy can be managed and progression slowed through proper blood sugar control, diet, exercise, and weight loss. However, damage to the retina is usually permanent. Once the disease advances to later stages, it cannot be reversed. This is why early detection is critical.
What are the warning signs of diabetic eye problems?
Many diabetic eye diseases show no symptoms in early stages. Warning signs that require immediate attention include: spots or floaters in your vision, blurred or distorted vision, sudden vision changes, dark or empty areas in your vision, difficulty reading, and seeing halos around lights. Contact an eye care professional immediately if you experience any of these symptoms.
Does insurance cover eye exams for people with diabetes?
Yes, medical insurance typically covers comprehensive eye exams for people with diabetes. You don’t need separate vision insurance to get annual checkups. Diabetic eye exams are considered preventive medical care, making regular monitoring more accessible and affordable.
How much vision loss from diabetes is preventable?
Approximately 90 percent of diabetes-related vision loss can be prevented with early detection and proper management. However, about 50 percent of people with diabetes don’t get the recommended annual eye exams. Early detection is crucial because damage often occurs before you notice any symptoms.
What Can You Do to Protect Your Vision?
Schedule Annual Dilated Eye Exams
A yearly dilated eye exam with an eye care professional is recommended for everyone with diabetes, even if your vision seems fine. For pregnant women with diabetes, additional eye exams throughout pregnancy may be necessary.
Manage Your Diabetes
- Monitor your blood sugar levels regularly
- Follow your prescribed diet and exercise plan
- Take medications or insulin as directed
- Work toward maintaining healthy blood sugar and hemoglobin A1C levels
Control Related Health Factors
- Manage blood pressure
- Keep cholesterol levels in check
- Maintain a healthy weight
- Exercise regularly (aim for at least 150 minutes of moderate aerobic activity weekly)
Know the Warning Signs
Contact a medical professional right away if you experience:
- Spots or dark strings floating in your sight (floaters)
- Blurred or spotty vision
- Sudden vision changes
- Dark or empty areas in your vision
- Vision loss
Don’t wait for vision problems to schedule your exam
Diabetes significantly impacts eye health, but you’re not powerless. With proper diabetes management and regular comprehensive eye exams, you can dramatically reduce your risk of vision loss. Your eye doctor can detect diabetes-related changes before you notice symptoms, making early intervention possible. Schedule a comprehensive eye examination with one of our experienced ophthalmologists in Charlotte at Horizon Eye Care.