Medically reviewed by
Krishna Patel, OD
If you’ve noticed your vision getting progressively blurrier despite frequent prescription changes, or if your teenager complains that their glasses never seem quite right anymore, keratoconus might be the reason why. This progressive eye condition affects the cornea, the clear, dome-shaped front surface of your eye, and while it can be concerning to hear the diagnosis, understanding keratoconus is the first step toward protecting your vision.
What Is Keratoconus?
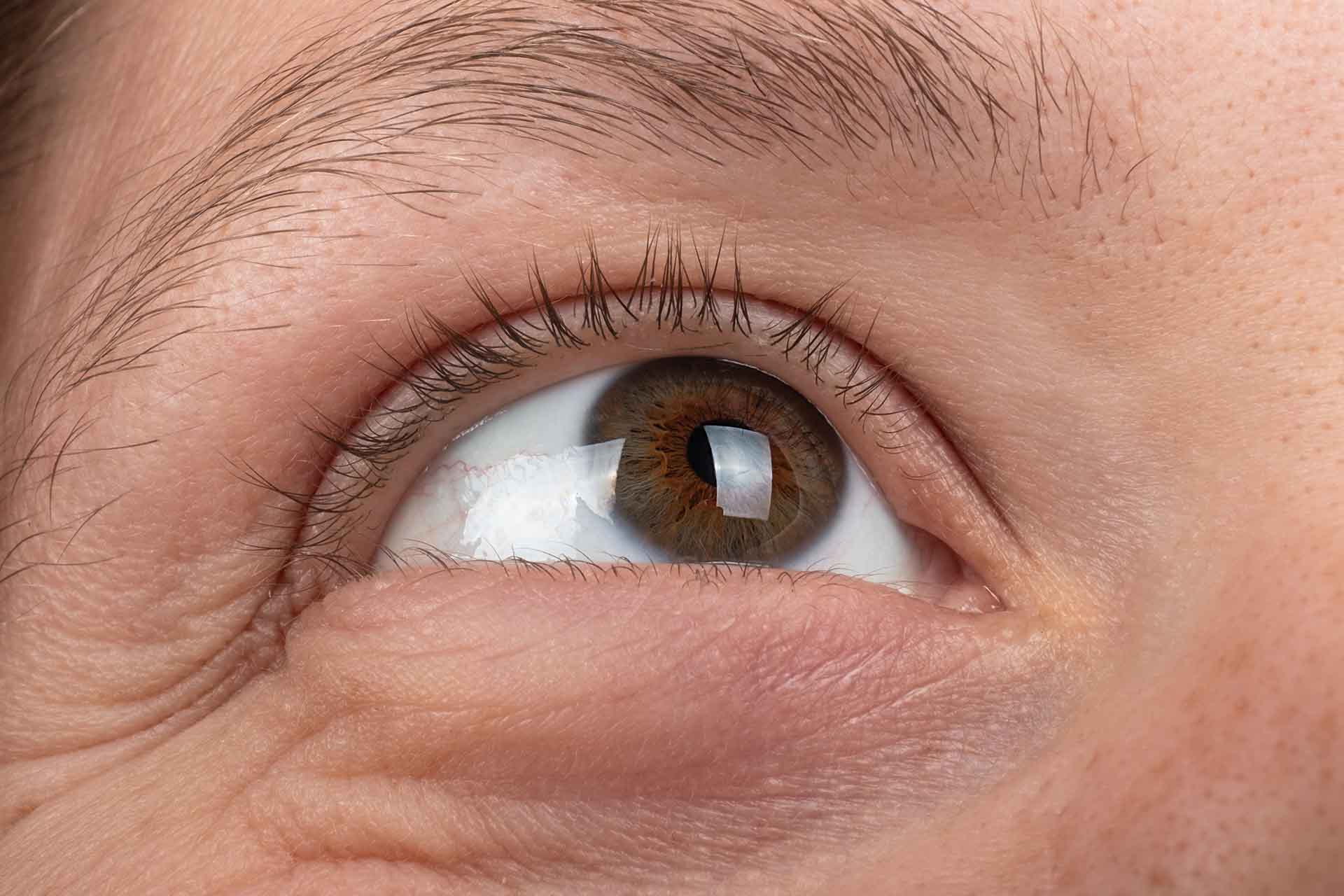
Keratoconus (pronounced ker-uh-toh-KOH-nus) occurs when the normally round cornea gradually thins and begins to bulge outward into a cone shape. Think of it like a soccer ball slowly developing a weak spot that pushes outward, this irregular shape prevents light from focusing properly on the retina, causing distorted and blurred vision.
The condition typically begins during the teenage years or early twenties, though it can start later. It usually affects both eyes, although one eye is often more severely affected than the other. The progression varies significantly from person to person, some experience only mild vision changes that stabilize on their own, while others see more rapid progression that requires intervention.
Recognizing the Signs
Keratoconus symptoms often develop gradually, which is why the condition sometimes goes undiagnosed initially. Watch for these warning signs:
Vision Changes:
- Blurred or distorted vision that glasses don’t fully correct
- Increased sensitivity to light and glare
- Halos or streaking around lights, especially at night
- Frequent prescription changes (every six months to a year)
- Difficulty driving at night
Other Symptoms:
- Eye irritation or excessive eye rubbing
- Sudden worsening of vision in one eye
- Difficulty with tasks requiring sharp vision, like reading road signs
For parents, pay attention if your teen suddenly struggles with activities that were previously easy, like reading the board at school, playing sports, or driving, especially if new glasses don’t seem to help much.
Why Does Keratoconus Happen?
The exact cause of keratoconus isn’t fully understood, but research has identified several contributing factors:
Genetic Connection: About 10% of people with keratoconus have a family member with the condition. If keratoconus runs in your family, earlier and more frequent eye exams can catch changes sooner.
Eye Rubbing: Chronic, vigorous eye rubbing appears to contribute to corneal damage. If you have allergies or conditions that make your eyes itch, managing those symptoms and avoiding rubbing is important.
Associated Conditions: Keratoconus is more common in people with certain systemic conditions, including Down syndrome, Ehlers-Danlos syndrome, and osteogenesis imperfecta. It’s also associated with chronic eye inflammation from conditions like allergic conjunctivitis.
How Keratoconus Progresses
Understanding how keratoconus typically progresses can help you and your eye doctor make informed decisions about treatment timing:
Early Stage: Mild astigmatism develops, often correctable with glasses or soft contact lenses. Vision changes are subtle and may be attributed to normal prescription changes.
Moderate Stage: The cornea continues to thin and bulge, causing more significant astigmatism. Standard glasses become less effective, and specialized contact lenses may be needed.
Advanced Stage: Severe corneal thinning and distortion create substantial vision impairment. Specialized contact lenses become necessary, and in some cases, corneal transplant may be considered.
The good news? Most people with keratoconus don’t progress to advanced stages, especially with early detection and appropriate treatment. The condition also tends to stabilize as people reach their 40s.
Treatment Options: From Conservative to Advanced
Modern treatment for keratoconus focuses on two goals: improving vision and stopping progression. Your cornea specialist will recommend options based on the severity of your condition and how quickly it’s changing.
Glasses and Contact Lenses
For Early Keratoconus: Standard prescription glasses or soft contact lenses can correct vision effectively in the early stages when corneal irregularity is mild.
For Moderate Keratoconus: As the cornea becomes more irregular, specialized contact lenses provide better vision:
- Rigid Gas Permeable (RGP) Lenses: These hard lenses create a new, smooth refracting surface over the irregular cornea, providing clearer vision than glasses.
- Scleral Lenses: These larger lenses vault over the entire cornea and rest on the white part of the eye (sclera). They’re often more comfortable than RGP lenses and provide excellent vision correction even for advanced keratoconus.
- Hybrid Lenses: Combining a rigid center with a soft outer ring, these lenses offer the vision clarity of hard lenses with improved comfort.
Many patients achieve excellent vision with specialty contact lenses and never need additional treatment. However, contacts address the symptom (blurred vision) without stopping the underlying progression.
Corneal Cross-Linking (CXL)
This treatment actually stops keratoconus from getting worse, something glasses and contacts cannot do. Corneal cross-linking strengthens the corneal tissue by creating new bonds between collagen fibers, much like adding supports to reinforce a structure.
The Procedure: During cross-linking, vitamin B2 (riboflavin) drops are applied to the cornea, which is then exposed to controlled UV light. This combination triggers a chemical reaction that strengthens corneal tissue. The procedure takes about an hour and is performed in the office.
Who Benefits: Cross-linking is most effective for patients showing documented progression, meaning the cornea is actively thinning and bulging. It’s particularly valuable for younger patients diagnosed with keratoconus, as it can prevent years of worsening vision.
What to Expect: Recovery typically takes a few days to a week, with some discomfort and light sensitivity during healing. Vision may fluctuate initially but often stabilizes or even improves slightly over several months as the cornea strengthens.
Intacs: Corneal Ring Segments
For patients with moderate keratoconus who don’t achieve adequate vision with contacts, tiny curved implants called Intacs can be inserted into the cornea to help flatten the cone and improve the corneal shape. These semi-circular plastic rings are placed in the outer cornea to provide structural support and reduce irregular astigmatism.
Intacs can improve vision quality and may reduce dependency on specialty contact lenses, though many patients still benefit from wearing contacts after the procedure for optimal vision.
Corneal Transplant
When keratoconus is very advanced and other treatments haven’t maintained functional vision, a corneal transplant (keratoplasty) may be necessary. During this procedure, the damaged cornea is replaced with healthy donor tissue.
Modern techniques, including partial-thickness transplants that replace only the damaged layers of the cornea, have improved outcomes and recovery times. However, transplant is typically reserved for the small percentage of patients who cannot achieve adequate vision through other means.
Why Early Detection Changes Everything
Catching keratoconus early makes a significant difference in long-term outcomes. Here’s why:
Treatment Is Most Effective Early: Corneal cross-linking works best when performed before significant thinning occurs. Stopping progression early means better preserved vision and potentially avoiding more invasive treatments later.
Better Vision Outcomes: Patients diagnosed and treated early often maintain better vision throughout their lives, with less dependence on complex contact lens fittings or surgical interventions.
More Treatment Options: In early stages, you have the full range of treatment options available. As keratoconus advances, some options become less effective.
Reduced Lifetime Cost: While specialty contact lenses and treatments have upfront costs, early intervention can prevent more expensive procedures like transplants and reduce the lifetime cost of managing the condition.
Living Well with Keratoconus
A keratoconus diagnosis can feel overwhelming, but most people with the condition live full, active lives with good functional vision. Here are some practical tips:
Protect Your Eyes:
- Manage allergies aggressively to reduce eye itching and rubbing
- If you must touch your eyes, use a gentle dabbing motion rather than rubbing
- Wear sunglasses to reduce light sensitivity and protect your eyes
- Use lubricating eye drops if your eyes feel dry or irritated
Stay Connected with Your Eye Care Team:
- Attend regular monitoring appointments, especially in the first few years after diagnosis
- Report any sudden vision changes immediately
- Be patient with contact lens fittings, finding the right fit can take time
- Ask questions about new treatment options as they become available
Build Your Support Network:
- Connect with other people who have keratoconus through support groups
- Educate family members and close friends about your condition
- Work with your school or employer if you need accommodations
Plan Ahead:
- Allow extra time for tasks requiring clear vision
- Have backup glasses even if you primarily wear contacts
- Keep good lighting in your work and living spaces
- Schedule important visual tasks (like driving in unfamiliar places) for times when your vision is clearest
Questions to Ask Your Cornea Specialist
If you’ve been diagnosed with keratoconus or suspect you might have it, these questions can guide your conversation with your eye doctor:
- How advanced is my keratoconus, and is it progressing?
- What treatment options are appropriate for my specific case?
- If I need specialty contact lenses, what type would work best for my lifestyle?
- Am I a candidate for corneal cross-linking?
- How often should I be monitored?
- What signs should prompt me to call your office between appointments?
- Are there any lifestyle changes that could help protect my vision?
- What should I tell my family members about screening?
When to Seek Care
Schedule a comprehensive eye exam if you experience:
- Progressively blurry vision that glasses don’t fully correct
- Frequent prescription changes (more than once a year)
- Increased sensitivity to light or glare
- Distorted vision or halos around lights
- Difficulty with night driving
- A family history of keratoconus
Seek same-day care if you experience sudden vision loss or a sudden increase in haziness, these could indicate corneal swelling (hydrops) that requires prompt attention.
Hope and Perspective
Twenty years ago, a keratoconus diagnosis meant a high likelihood of eventually needing a corneal transplant. Today, with earlier detection, corneal cross-linking to halt progression, and advanced contact lens designs, most patients maintain functional vision throughout their lives without requiring transplant surgery.
Research continues to advance our understanding of keratoconus. New treatments and technologies are in development, and genetic research may one day help us prevent the condition entirely in at-risk individuals.
If you’re living with keratoconus, remember that you’re not alone, an estimated 1 in 2,000 people have the condition, and that number may be higher as diagnostic technology improves. With proper care and monitoring, most people with keratoconus continue doing the things they love, from reading to driving to pursuing their careers.
Expert Cornea Care in Charlotte
At Horizon Eye Care, our cornea specialists have extensive experience diagnosing and managing keratoconus. We utilize advanced diagnostic imaging to detect even subtle corneal changes and offer the full spectrum of treatment options, from specialty contact lens fittings to corneal cross-linking.
If you’re experiencing vision changes or have concerns about keratoconus, we’re here to provide the expert care and personalized attention you deserve. Early evaluation makes all the difference in protecting your vision for the long term.
Ready to take the next step? Contact Horizon Eye Care at 704-365-0555 to schedule a consultation with one of our cornea specialists. We have seven convenient locations throughout the Charlotte area, and we’re here to answer your questions and provide the clarity you need, both literally and figuratively.
The information provided in this blog is for educational purposes and should not replace professional medical advice. If you’re experiencing vision changes, please schedule an appointment with an eye care professional for a comprehensive evaluation.