Medically reviewed by
Benjamin C. Kramer, MD
Pediatricians and psychologists can debate exactly when childhood ends, but the eyes have their own idea. By the age of 7 or 8, your brain and eyes enter a relationship that won’t change much. If parents don’t seek pediatric eye care to quickly address vision problems, especially the one known as “lazy eye,” they may be forever too late.
Kids seldom suffer from most of the eye problems that affect adults: dry eye, glaucoma, corneal issues or many others. However, two conditions crop up frequently in childhood that need to be addressed quickly. Ophthalmologists can look for them at any age from infancy onward.

Two Conditions to Watch For: Strabismus and Amblyopia
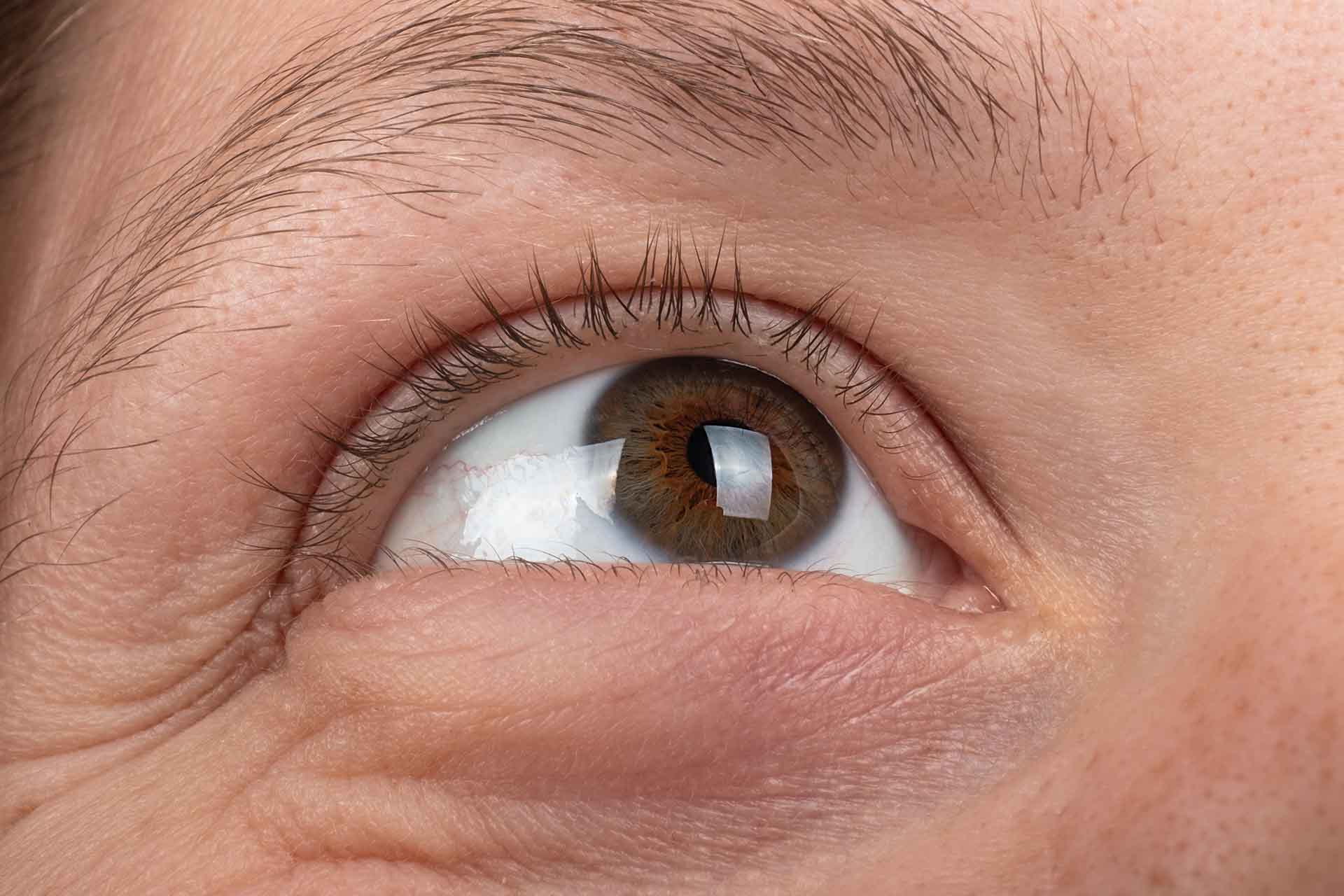
Strabismus (Misaligned Eyes)
Parents will often detect the first on sight. Strabismus makes the eyes deviate when looking at an object, turning them inward or outward away from the center. This condition, sometimes called “wandering eye,” can be constant or intermittent but does not fix itself.
How Common Is Strabismus?
Strabismus affects approximately 3 to 4 percent of children, making it one of the most common pediatric eye conditions. The prevalence varies slightly across different populations and age groups, with some studies reporting rates between 2.5 and 7 percent depending on the type of strabismus and the population studied.
Strabismus Treatment Options
Doctors often address it with prescription eyeglasses, which force the eyes to look straight ahead. (Eyes may wander again when glasses aren’t worn.) If this doesn’t fix the problem, surgery can promote proper vision and alignment. Modern strabismus surgery has excellent outcomes, with success rates of approximately 74 percent for achieving proper eye alignment within 10 degrees or less of normal position in young children.
Untreated strabismus can last into adulthood, where it may involve complications such as double vision and loss of depth perception. It can also lead to the second problem, amblyopia. Beyond the medical concerns, strabismus can significantly impact a child’s quality of life, affecting self-esteem, social interactions, and even academic performance. Studies show that corrective surgery improves not just eye alignment, but also psychological well-being, reducing anxiety and depression in affected children.
Surgery Is Safer Than You Might Think
Many parents worry about their child undergoing eye surgery, but strabismus surgery performed under general anesthesia is one of the safest pediatric procedures. The surgery typically takes about one hour, and most children return to normal activities within a few days. Serious complications are rare, and the psychosocial benefits of early correction can be substantial.
Amblyopia (Lazy Eye)
This condition, known as “lazy eye,” is the most common cause of visual impairment among children receiving pediatric eye care in Charlotte: Between 2 and 3 out of every 100 children suffer from it. Amblyopia occurs when one eye doesn’t focus as well as the other; it may be significantly more nearsighted, more farsighted, or have more astigmatism. The brain gets clear images from one eye and cloudy pictures from the other, so it devotes all its attention to input from the good eye.
Why Does Amblyopia Develop?
The visual system develops rapidly during the first year of life, with vision becoming the dominant sense by 6 months of age. However, maturation of the visual system continues for several years. From birth to about 6 to 8 years of age, the visual system is susceptible to conditions that cause either blurred visual input or abnormal binocular interaction. When one eye consistently sends clearer images to the brain than the other, the brain essentially “shuts off” the weaker eye to avoid confusion.
Children Adjust Quickly to Amblyopia
They may succeed at sports or in a classroom, because they learn to rely only on that good eye. But the brain stops forming connections with the weak one after a certain time, often around the age of 8. After that, attempts to make the brain process images from the bad eye usually fail, though recent research shows some degree of improvement is possible even in older children and adults with intensive treatment.
Why Age Matters
The critical period for visual development can be divided into distinct phases that determine how effectively amblyopia can be treated.
Peak Sensitivity (Birth to 3 years)
When the visual system is most vulnerable to developing amblyopia and simultaneously most responsive to treatment. Success rates when treatment begins before age 3 can exceed 90 percent, with many children achieving normal or near-normal vision.
Declining Sensitivity (3 to 7 years)
Treatment remains highly effective but may require longer duration and more intensive approaches. Success rates between ages 3 and 5 remain excellent, ranging from 75 to 80 percent for achieving good visual outcomes. Between ages 5 and 7, success rates are approximately 60 to 75 percent with standard therapies.
Extended Sensitivity (7 to 12 years)
Some degree of brain plasticity remains, allowing for treatment with variable success rates. Children aged 7 to 13 are significantly less responsive to treatment compared with younger age groups, though meaningful improvements are still possible. Studies show that even after age 7, about 50 to 60 percent of children can achieve significant visual improvement with treatment.
How Doctors Treat Amblyopia
Doctors who catch amblyopia early can treat it by patching the good eye or putting drops in it to blur the vision, forcing the brain to rely on the “lazy” eye. The most common approaches include:
Optical Correction (Glasses)
In a proportion of children, amblyopia will completely resolve with glasses alone. Wearing appropriate glasses corrects refractive errors and can improve amblyopia by 25 percent in children aged 7 to 12 years through optical correction alone, before any other treatment begins.
Patching Therapy
The gold standard treatment involves covering the stronger eye with a patch for a prescribed number of hours each day, combined with near-vision activities like reading, coloring, or playing video games. The key to success is compliance. Studies show that treatment success rates increase in proportion to the actual hours of patch wear, up to a level where visual acuity plateaus.
Atropine Eye Drops
An alternative to patching, atropine drops temporarily blur vision in the good eye, forcing the brain to use the amblyopic eye. Success rates with atropine are similar to patching (50 to 80 percent), and some studies suggest it may be equally or more effective than patching for certain age groups and levels of amblyopia.
Duration of Treatment
Treatment typically continues until visual acuity equalizes between the two eyes or stops improving, which can take months to years depending on the severity of amblyopia and the child’s age. Most improvement occurs within the first 5 weeks of consistent treatment.
Risk of Recurrence
Even after successful treatment, approximately 24 percent of children may experience some recurrence of amblyopia, especially if treatment is stopped abruptly. Recurrence is more common during the first 13 weeks after cessation of treatment. Gradually tapering treatment rather than stopping suddenly can reduce the risk of regression.
But Left Alone, Amblyopia Persists
Amblyopia remains the most common cause of monocular (one-eyed) visual impairment among young and middle-aged adults. Data suggests that approximately 80 percent of childhood amblyopia persists beyond 16 years of age if left untreated. This may be due to failure of detection, lack of response to the original treatment, acuity loss following cessation of treatment, or only partial remediation of the amblyopia.
Long-Term Consequences
Untreated amblyopia can negatively impact school performance, self-esteem, employment prospects, functional skills, quality of life, future social interactions, and overall risk of blindness. Furthermore, people with amblyopia have an increased risk of their good eye becoming visually impaired from trauma or disease. The estimated lifetime risk of visual impairment in the sound eye is at least 1.2 to 3.3 percent, which means that maintaining the best possible vision in both eyes is crucial for long-term visual health.
It’s Never Too Early For an Exam
Pediatricians and school nurses often turn up vision problems and recommend patients to Horizon. Sometimes our Charlotte ophthalmologists conduct the first eye exam a youngster has ever had. Those can be valuable, even if eyes look normal and children don’t complain of blurry vision.
Recommended Eye Screening Schedule for Children
The American Academy of Pediatrics (AAP) and the American Academy of Ophthalmology (AAO) recommend that all children have an eye exam during the newborn period and again at all routine well-child visits. The U.S. Preventive Services Task Force specifically recommends screening to detect lazy eye (amblyopia), misaligned eyes (strabismus), and defects in visual acuity in children between the ages of 3 and 5 years, as this is when amblyopia is most treatable.
More specifically:
- Birth to 2 years: Eye exam at 6 to 12 months of age for asymptomatic, low-risk children. Earlier or more frequent exams for children with risk factors.
- Ages 3 to 5 years: Vision screening at least once, ideally annually, to detect amblyopia or its risk factors. This is the critical window for amblyopia detection and treatment.
- Ages 6 to 18 years: Screening before first grade and then every 1 to 2 years, or annually if risk factors are present.
Children at Higher Risk
Some children should bypass routine screening and receive a comprehensive eye examination from an eye care specialist. At-risk conditions include:
- Family history of childhood eye problems, especially genetic eye diseases
- Prematurity or low birth weight
- Developmental delays or neurological conditions
- Systemic medical conditions like diabetes or juvenile arthritis
- Previous eye injury or surgery
- Observable eye abnormalities like strabismus or drooping eyelids
Examining Young Children
Healthy youngsters may need to see an eye doctor only once every two or three years, depending on what’s discovered at the initial check-up. Even pre-verbal children can be assessed via toys and play activities to establish a baseline. Modern pediatric eye exams use age-appropriate techniques:
- Infants and Toddlers: Specialized instruments and observation tools assess eye health without requiring verbal responses. Tests might include checking how well the baby tracks moving objects, assessing pupil reactions, and using instruments that can objectively measure refractive error.
- Preschool Children: Testing may involve matching games, cartoons, or recognizable symbols like LEA Symbols (house, apple, circle, square) or HOTV letters. These make testing engaging for young children while providing accurate measurements.
- School-Age Children: Older children can participate in traditional eye chart testing along with comprehensive evaluation of eye health, focusing ability, and binocular vision.
It’s Never Too Early, But It Can Be Too Late
It’s never too early to get a thorough exam, followed by treatment where needed. But as patients who wait to address amblyopia know, some diagnoses come too late. The visual system’s critical period doesn’t wait for convenience, and the window for optimal treatment closes as children grow.
Early Detection Changes Lives
Vision is fundamental to a child’s development, affecting their ability to learn, play, and interact with the world. Most pediatric vision problems are highly treatable when caught early. Strabismus surgery can restore eye alignment and improve quality of life. Amblyopia treatment can preserve vision in the weaker eye, protecting against future vision loss and maintaining depth perception.
What Parents Can Do
- Watch for warning signs: Eyes that don’t align properly, squinting, head tilting, sitting too close to the TV, covering one eye, or complaints of blurred vision
- Don’t wait for symptoms: Many serious pediatric eye conditions show no obvious signs, especially amblyopia
- Follow screening recommendations: Ensure your child receives age-appropriate vision screenings
- Act quickly if problems are detected: The earlier treatment begins, the better the outcomes
- Complete the full treatment course: Stopping treatment too soon can lead to regression of improvements
At Horizon Eye Care, our fellowship-trained pediatric ophthalmologists understand that children aren’t just small adults. They require specialized techniques, patience, and age-appropriate approaches. From newborns to teenagers, we provide comprehensive eye care designed specifically for young patients.